Frequency
Hypochromic microcytic anemia with iron overload is likely a rare disorder; at least five affected families have been reported in the scientific literature.
Causes
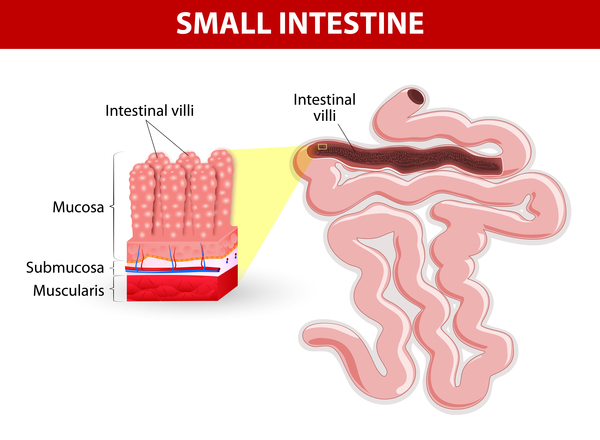
Mutations in the SLC11A2 gene cause hypochromic microcytic anemia with iron overload. The SLC11A2 gene provides instructions for making a protein called divalent metal transporter 1 (DMT1). The DMT1 protein is found in all tissues, where its primary role is to transport positively charged iron atoms (ions) within cells. In a section of the small intestine called the duodenum, the DMT1 protein is located within finger-like projections called microvilli. These projections absorb nutrients from food as it passes through the intestine and then release them into the bloodstream. In all other cells, including immature red blood cells called erythroblasts, DMT1 is located in the membrane of endosomes, which are specialized compartments that are formed at the cell surface to carry proteins and other molecules to their destinations within the cell. DMT1 transports iron from the endosomes to the cytoplasm so it can be used by the cell.
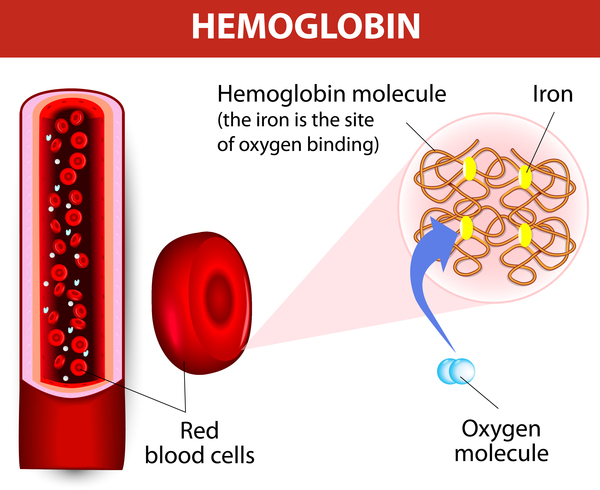
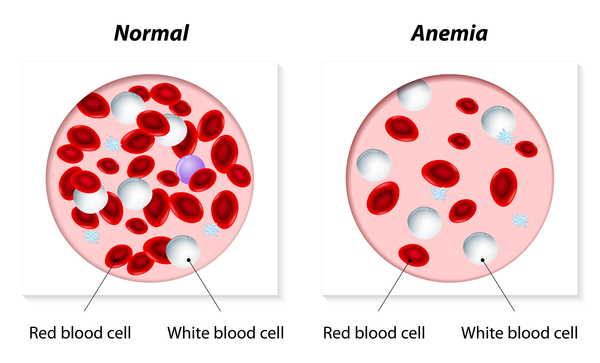
SLC11A2 gene mutations lead to reduced production of the DMT1 protein, decreased protein function, or impaired ability of the protein to get to the correct location in cells. In erythroblasts, a shortage of DMT1 protein diminishes the amount of iron transported within cells to attach to hemoglobin. As a result, the development of healthy red blood cells is impaired, leading to a shortage of these cells. In the duodenum, a shortage of DMT1 protein decreases iron absorption. To compensate, cells increase production of functional DMT1 protein, which increases iron absorption. Because the red blood cells cannot use the iron that is absorbed, it accumulates in the liver, eventually impairing liver function. The lack of involvement of other tissues in hypochromic microcytic anemia with iron overload is likely because these tissues have other ways to transport iron.
Inheritance
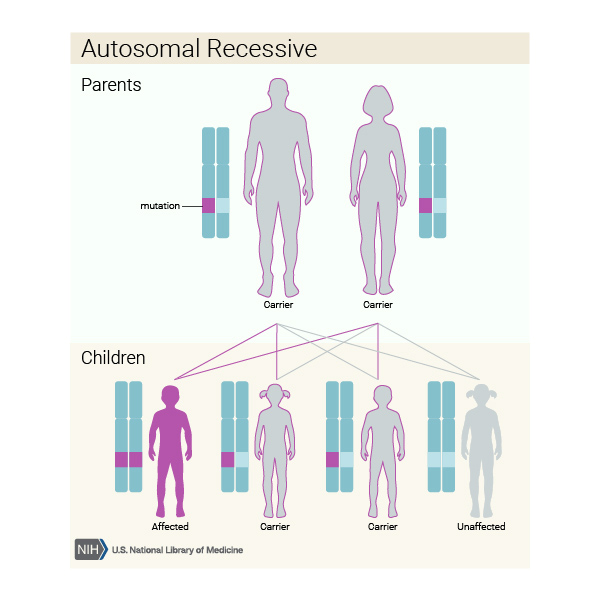
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Other Names for This Condition
- Microcytic anemia and hepatic iron overload
- Microcytic anemia with liver iron overload
Additional Information & Resources
Genetic Testing Information
Genetic and Rare Diseases Information Center
Patient Support and Advocacy Resources
Catalog of Genes and Diseases from OMIM
Scientific Articles on PubMed
References
- Bardou-Jacquet E, Island ML, Jouanolle AM, Detivaud L, Fatih N, Ropert M, Brissot E, Mosser A, Maisonneuve H, Brissot P, Loreal O. A novel N491S mutation in the human SLC11A2 gene impairs protein trafficking and in association with the G212V mutation leads to microcytic anemia and liver iron overload. Blood Cells Mol Dis. 2011 Dec 15;47(4):243-8. doi: 10.1016/j.bcmd.2011.07.004. Epub 2011 Aug 26. Citation on PubMed
- Beaumont C, Delaunay J, Hetet G, Grandchamp B, de Montalembert M, Tchernia G. Two new human DMT1 gene mutations in a patient with microcytic anemia, low ferritinemia, and liver iron overload. Blood. 2006 May 15;107(10):4168-70. doi: 10.1182/blood-2005-10-4269. Epub 2006 Jan 26. Citation on PubMed
- Iolascon A, d'Apolito M, Servedio V, Cimmino F, Piga A, Camaschella C. Microcytic anemia and hepatic iron overload in a child with compound heterozygous mutations in DMT1 (SCL11A2). Blood. 2006 Jan 1;107(1):349-54. doi: 10.1182/blood-2005-06-2477. Epub 2005 Sep 13. Citation on PubMed
- Iolascon A, De Falco L. Mutations in the gene encoding DMT1: clinical presentation and treatment. Semin Hematol. 2009 Oct;46(4):358-70. doi: 10.1053/j.seminhematol.2009.06.005. Citation on PubMed
- Lam-Yuk-Tseung S, Camaschella C, Iolascon A, Gros P. A novel R416C mutation in human DMT1 (SLC11A2) displays pleiotropic effects on function and causes microcytic anemia and hepatic iron overload. Blood Cells Mol Dis. 2006 May-Jun;36(3):347-54. doi: 10.1016/j.bcmd.2006.01.011. Epub 2006 Apr 3. Citation on PubMed
The information on this site should not be used as a substitute for professional medical care or advice. Contact a health care provider if you have questions about your health.