Frequency
BLS II is a rare condition. At least 100 cases have been reported in the medical literature. While BLS II has been found in several populations throughout the world, it appears to be especially prevalent in the Mediterranean region and North Africa.
Causes
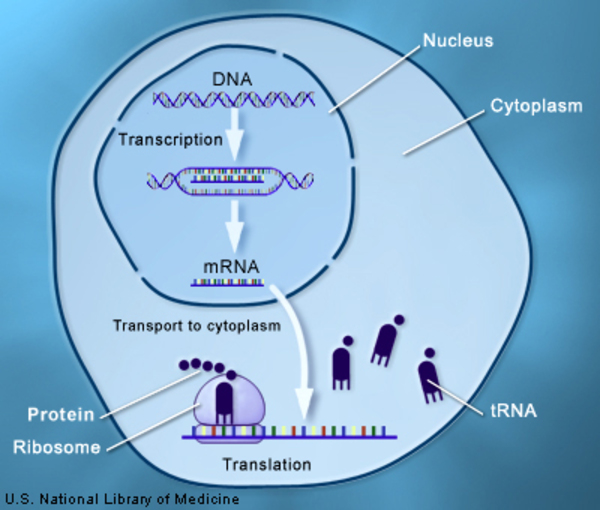
BLS II is caused by mutations in the CIITA, RFX5, RFXANK, or RFXAP gene. Each of these genes provides instructions for making a protein that plays a role in controlling the activity (transcription) of genes called MHC class II genes. Transcription is the first step in the production of proteins, and the CIITA, RFX5, RFXANK, and RFXAP proteins are critical for the production of MHC class II proteins from these genes.
The RFX5, RFXANK, and RFXAP proteins come together to form the regulatory factor X (RFX) complex, which attaches (binds) to specific regions of DNA involved in the regulation of MHC class II gene activity. The CIITA protein interacts with the RFX complex and brings together other proteins that turn on gene transcription, leading to the production of MHC class II proteins.
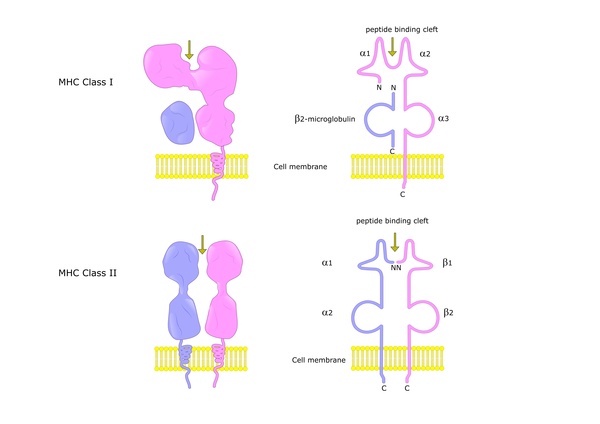
MHC class II proteins play an important role in the body's immune response to foreign invaders, such as bacteria, viruses, and fungi. To help the body recognize and fight infections, MHC class II proteins on lymphocytes bind to fragments of proteins (peptides) from foreign invaders so that other specialized immune system cells can interact with them. When these immune system cells recognize the peptides as harmful, they trigger the lymphocytes to launch immune responses to get rid of the foreign invaders.
Mutations in the CIITA, RFX5, RFXANK, or RFXAP gene prevent transcription of MHC class II genes, which leads to an absence of MHC class II proteins on the surface of certain lymphocytes. Lack of these proteins on lymphocytes impairs the body's immune response to bacteria, viruses, and fungi, leading to persistent infections in individuals with BLS II syndrome.
Inheritance
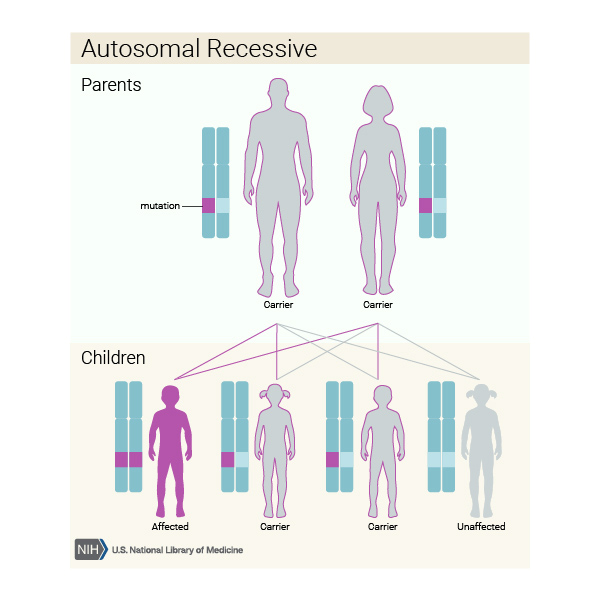
This condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
Other Names for This Condition
- Bare lymphocyte syndrome type 2
- BLS type II
- Major histocompatibility complex class II deficiency
- MHC class II deficiency
- SCID due to absence of class II HLA antigens
- SCID, HLA class 2-negative
- SCID, HLA class II-negative
- Severe combined immunodeficiency due to absent class II human leukocyte antigens
- Severe combined immunodeficiency, HLA class II-negative
Additional Information & Resources
Genetic and Rare Diseases Information Center
Patient Support and Advocacy Resources
Clinical Trials
Catalog of Genes and Diseases from OMIM
Scientific Articles on PubMed
References
- Ahmed A, Reith W, Puck JM, Cheng LE. Novel Mutation in the Class II Transactivator Associated with Immunodeficiency and Autoimmunity. J Clin Immunol. 2015 Aug;35(6):521-2. doi: 10.1007/s10875-015-0183-z. Epub 2015 Aug 14. No abstract available. Citation on PubMed
- Burd AL, Ingraham RH, Goldrick SE, Kroe RR, Crute JJ, Grygon CA. Assembly of major histocompatibility complex (MHC) class II transcription factors: association and promoter recognition of RFX proteins. Biochemistry. 2004 Oct 12;43(40):12750-60. doi: 10.1021/bi030262o. Citation on PubMed
- Garvie CW, Boss JM. Assembly of the RFX complex on the MHCII promoter: role of RFXAP and RFXB in relieving autoinhibition of RFX5. Biochim Biophys Acta. 2008 Dec;1779(12):797-804. doi: 10.1016/j.bbagrm.2008.07.012. Epub 2008 Aug 6. Citation on PubMed
- Gobin SJ, Peijnenburg A, van Eggermond M, van Zutphen M, van den Berg R, van den Elsen PJ. The RFX complex is crucial for the constitutive and CIITA-mediated transactivation of MHC class I and beta2-microglobulin genes. Immunity. 1998 Oct;9(4):531-41. doi: 10.1016/s1074-7613(00)80636-6. Citation on PubMed
- Saleem MA, Arkwright PD, Davies EG, Cant AJ, Veys PA. Clinical course of patients with major histocompatibility complex class II deficiency. Arch Dis Child. 2000 Oct;83(4):356-9. doi: 10.1136/adc.83.4.356. Citation on PubMed or Free article on PubMed Central
- Shrestha D, Szollosi J, Jenei A. Bare lymphocyte syndrome: an opportunity to discover our immune system. Immunol Lett. 2012 Jan 30;141(2):147-57. doi: 10.1016/j.imlet.2011.10.007. Epub 2011 Oct 17. Citation on PubMed
The information on this site should not be used as a substitute for professional medical care or advice. Contact a health care provider if you have questions about your health.